Table of Contents
Introduction
With multiple locations across Southern California, our providers are ready to help you tackle your wound with an individualized treatment plan. For diabetics in particular, proper wound care is essential.
Know Your Wound
Our podiatrists will complete a thorough consultation and physical exam to diagnose your wound and determine its severity. This may include asking about your medical history, chronic health conditions, lifestyle, and any symptoms you’re experiencing.
We treat multiple wounds at our clinics, including diabetic, pressure, venous, and arterial/ischemic ulcerations, as well as ulcers. The sooner we know your exact wound, the quicker we can help manage it.
Wounds & Diabetes
Open wounds caused by diabetes are common, but we can help. As diabetes naturally slows down the healing process, open wounds on the lower extremities can quickly become non-healing wounds. As such, what may start as a small wound could snowball into more severe foot complications if left untreated.
Diabetics need to inspect their feet daily for wounds. They also need to routinely self-assess if they experience feeling in their feet. Neuropathy is a type of nerve damage that affects the body and causes lost feeling in the feet. As a result, a wound could develop, go unnoticed, and quickly become infected.
Treating Diabetic Wounds
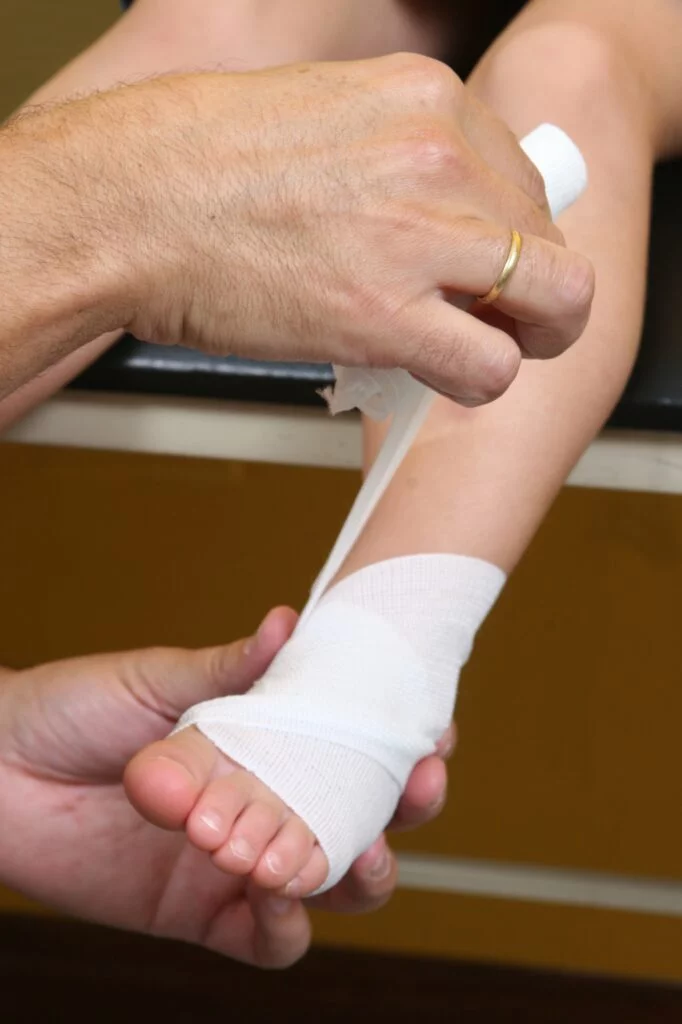
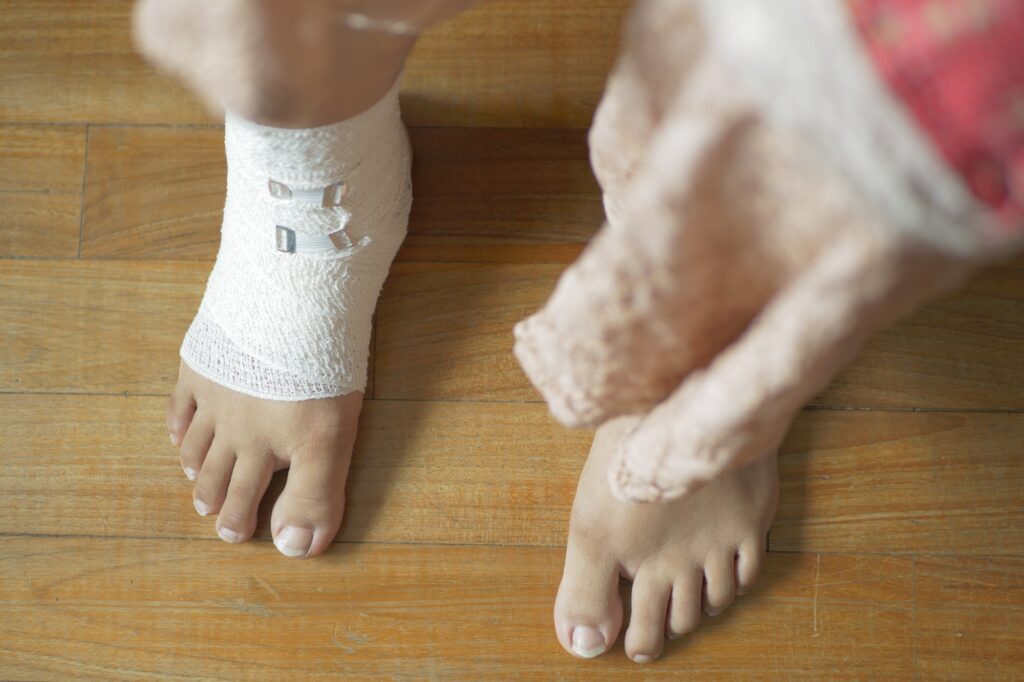
Once a diabetic wound is discovered, it should be treated as soon as possible by a podiatrist to avoid infection. Infection can lead to gangrene and increases your risk of limb loss. At your podiatrist visit, the wound will be cleaned with water only and removing any damaged or dead tissue from the area. Using soap or iodine can make the problem worse. Depending on the severity of the wound, antibiotic ointment will then be applied and covered with a bandage that should be changed daily.
Ulcers
Treating Ulcers
Wound Prevention
Some ways to prevent wounds from developing include:
- Checking your feet daily for any injuries
- Washing and drying your feet daily
- Wearing proper footwear (no shoes that are too tight)
- Trimming your toenails straight across