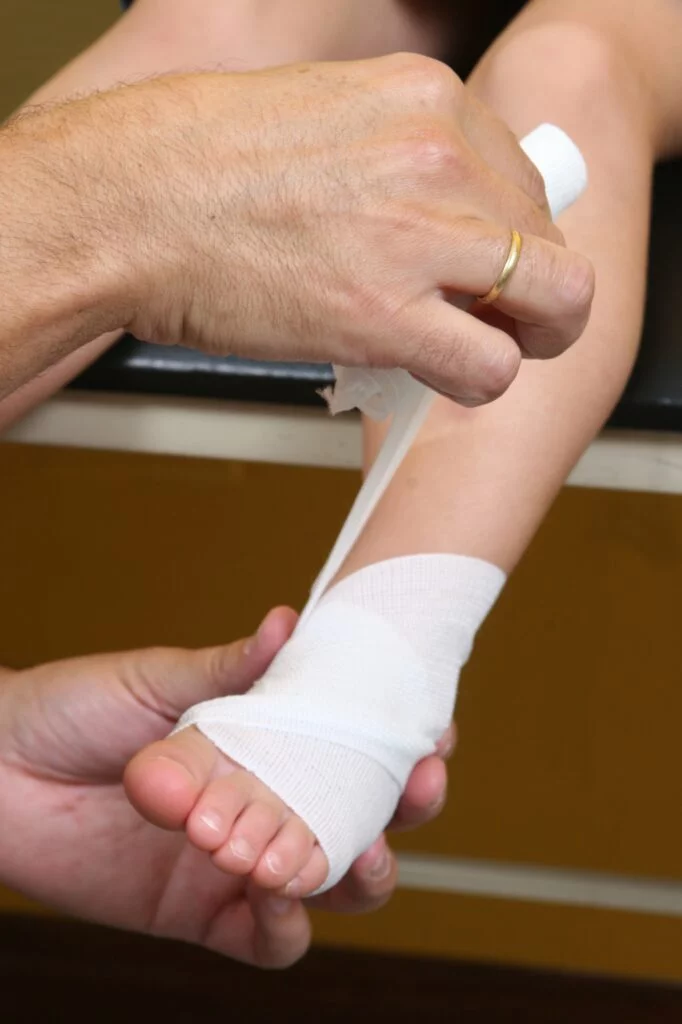
Thumb Arthritis
A joint is formed when two bones meet and articulate, which allows movement. Joints are lined with smooth cartilage that allows for the easy movement of one bone relative to another. Osteoarthritis, or degenerative arthritis, is a process that occurs with aging and describes the deterioration of the joint cartilage. Thumb arthritis is the second most common type of arthritis in the hand; the most prevalent hand arthritis involves the last joint in each finger.
Thumb arthritis is also known as basal joint arthritis. It is more common in women, though certainly men can develop this type of problem. Typically, degenerative arthritis of the thumb occurs sometime after 40 years of age. There is a genetic predisposition in developing this arthritis condition. Additionally, any type of trauma to the thumb can predispose one to thumb arthritis. There are other conditions such as inflammatory arthritis (Lupus, Rheumatoid Arthritis) that can affect the base of the thumb and cause the deterioration of that joint.
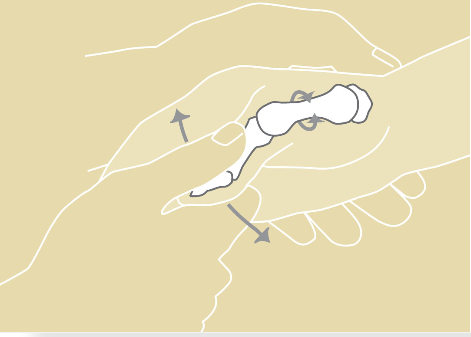
A grind test that your hand surgeon may perform to diagnose thumb arthritis
Signs and Symptoms
Activities which rely on the thumb may result in pain at the base of the thumb, particularly in an arthritic joint. The activities most people notice as painful include pinching, grasping or gripping. Signs and symptoms of thumb arthritis may include swelling or stiffness at the base of the thumb. As the arthritis progresses, the pain and weakness may increase along with decreasing range of motion at the base of the thumb. As the arthritis advances even further, bone spurs may develop, resulting in an enlarged appearance at the base of the thumb.
Diagnosis
If the pain starts to interfere with one’s activities of daily living, then a visit with a hand surgeon could be helpful. During a physical examination of an arthritic thumb, the physician may notice grinding when maneuvering the thumb in a certain way (see Figure 1). X-rays can be used to confirm the diagnosis.
Treatment
Treatment options are based on the severity of the symptoms. There is no convincing evidence to support the use of any medications or supplements to prevent the progression of thumb arthritis. X-rays show that basal joint arthritis will generally get worse with time. The rate of the progression of arthritis varies from one person to another. Even though thumb arthritis will advance with time, the symptoms do not always get worse, and in some people the symptoms will decrease significantly.
Nonoperative treatment for thumb arthritis can involve:
- Anti-inflammatory medications (consult your doctor first)
- The use of heat or ice
- Bracing
- Exercises
- Ergonomic adjustments
- Avoidance of irritating activities
- Steroid injections into the basal joint
- Occupational therapy
When nonoperative treatment fails and when the patient is sufficiently symptomatic, surgery is an option. Surgery can involve removing part or all of the trapezium (one of the bones in the thumb joint) and cushioning or suspending the thumb joint with a variety of possible techniques. Fusing (making the two bones into one) the thumb joint is also an option. The complete recovery after a thumb surgery can take anywhere between 8 weeks and one year.